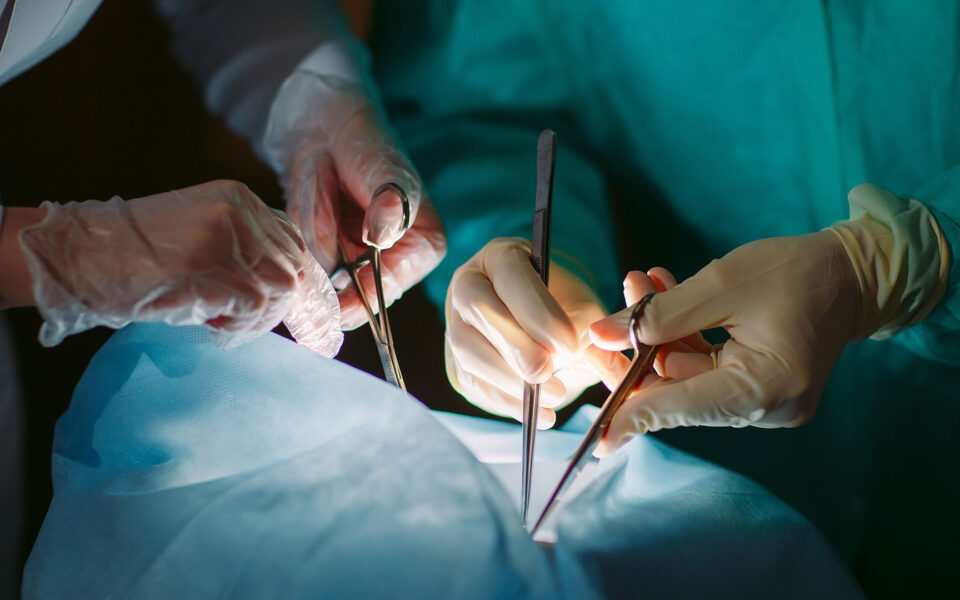
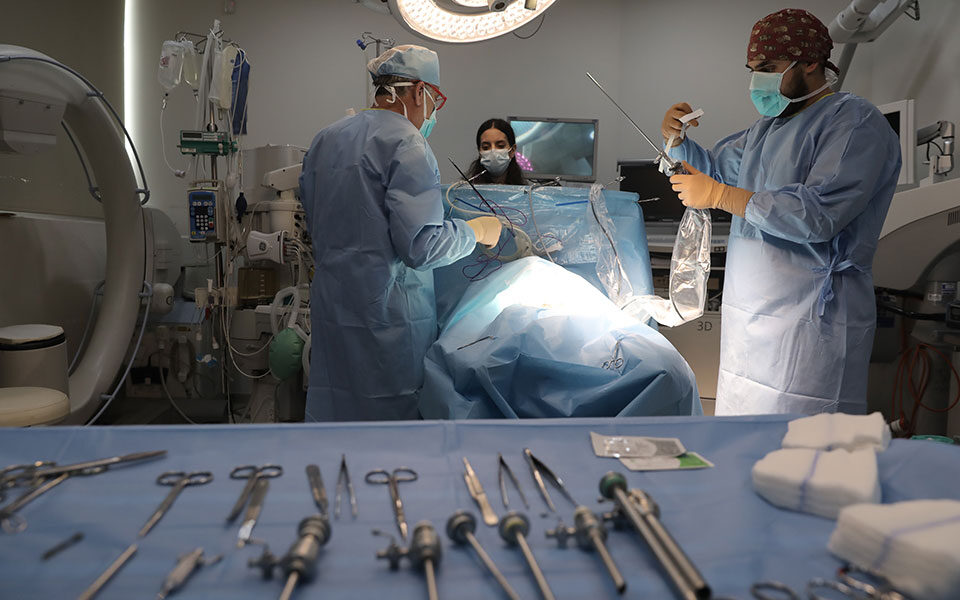
Australia’s lack of clear triage protocols puts lives at risk if another Covid crisis hits
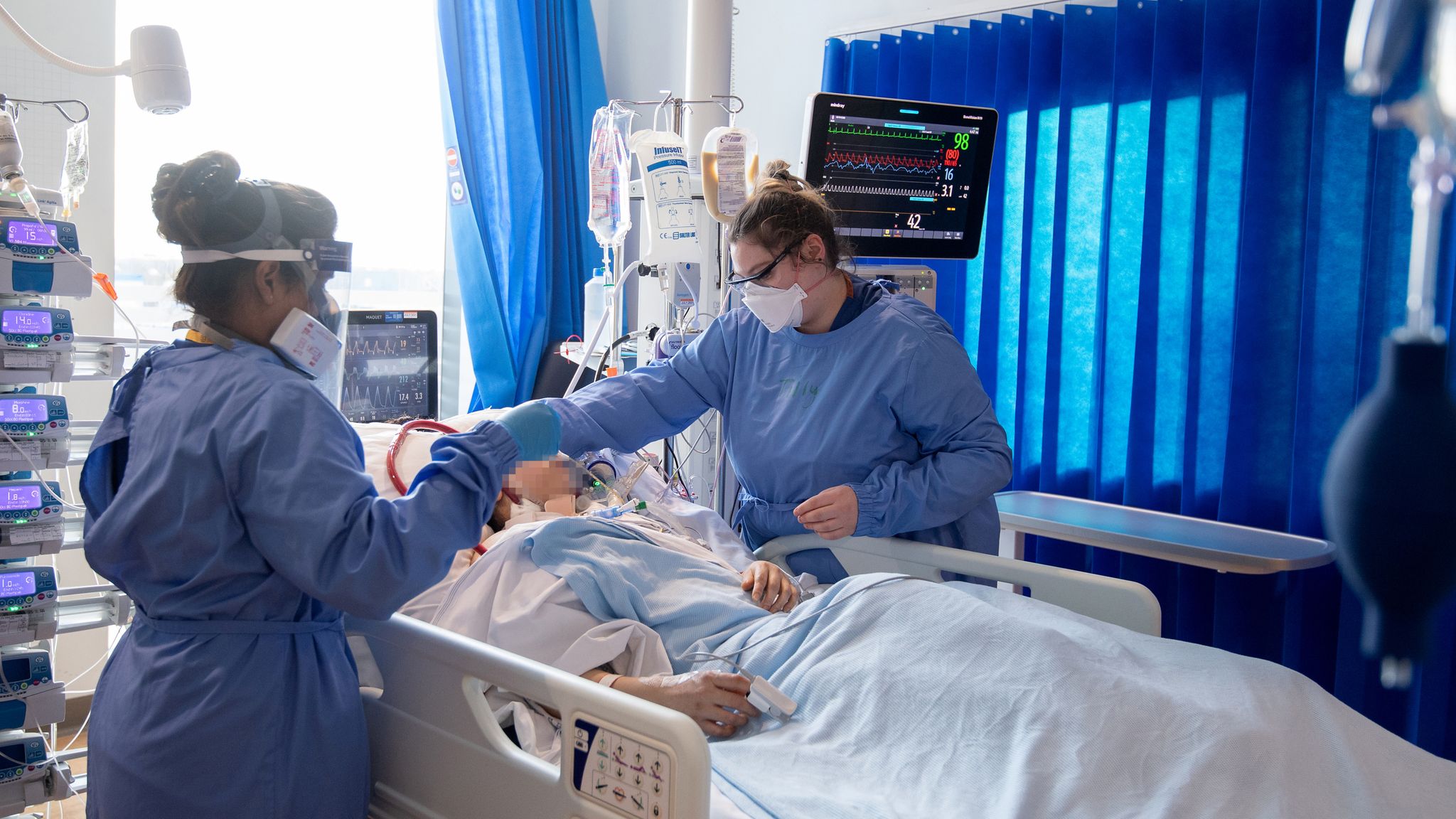

Australia’s lack of clear triage protocols more than a year into the Covid-19 pandemic means clinicians will struggle to decide which patients to save and how to treat them should the virus return, an analysis published in the Medical Journal of Australia has found.
Because Australia has avoided the scale of pandemic that has overwhelmed health systems elsewhere, federal and state governments have been reluctant to develop or make public triage protocols, the analysis, led by Dr Eliana Close from Queensland University of Technology’s Australian centre for health law research, said.
The study authors said waiting until crisis point carried significant risks.
“Public confidence is enhanced when governments have the political courage to embark on these difficult public debates in advance of need,” they said.
“Prioritising some individuals over others when the demand for resources exceeds supply is confronting for clinicians and the community alike, and challenges us to reflect on our deeply held values as a society.
“When clinicians are allocating scarce resources, they need standards to support their decisions which have been subject to public consultation and rigorous legal review.”
The president of the Australian Medical Association, Dr Omar Khorshid, has warned Covid “is coming” one way or another.
He said too many Australians assumed that because vaccination was under way and there was no community transmission, that would remain the case, with occasional short-lived lockdowns required should a hotel quarantine breach see the virus enter the community.
But he said: “Covid-19 is going to continue to come to Australia. Whether it’s through a breach of our quarantine or because we open the borders, it is coming.
“There is no way for Australia to avoid Covid unless we close ourselves off forever.
“But that’s that’s not going to be acceptable. So Covid will come, because there is just no way to eradicate this virus from the entire globe. There’s such vaccine inequity that we’re going to have virus hotspots, with huge amounts of devastating Covid for a long period of time.
“And we are going to have to manage that risk with open borders through mechanisms such as vaccination, quarantine, and a boosted health system which is going to have to learn to manage people with Covid.”
Khorshid said although many Australians would be vaccinated, new variants combined with possible waning immunity over time meant Australians could not expect there would never be outbreaks.
“From time to time it will happen, because once the virus comes into our community there’s going to be people who haven’t been vaccinated or who haven’t had an immune response to the vaccine,” he said.
“So we need to be able to have a health system able to manage the extra burden of disease that will come with Covid.
“And of course we haven’t had the flu for the last couple of years due to the measures we have had in place for Covid. So we also need to prepare the health system for a surge in those cases too, and to encourage flu vaccination.”
On Tuesday the AMA federal council warned that the health system was not prepared for a serious Covid outbreak. If Australia was to confidently reopen international borders, it needed to ensure a high proportion of Australians were vaccinated and that the public hospitals had sufficient surge capacity available to deal with future community outbreaks.
Source: The Guardian