One in three people in the NSW hospitals with COVID-19 is in intensive care
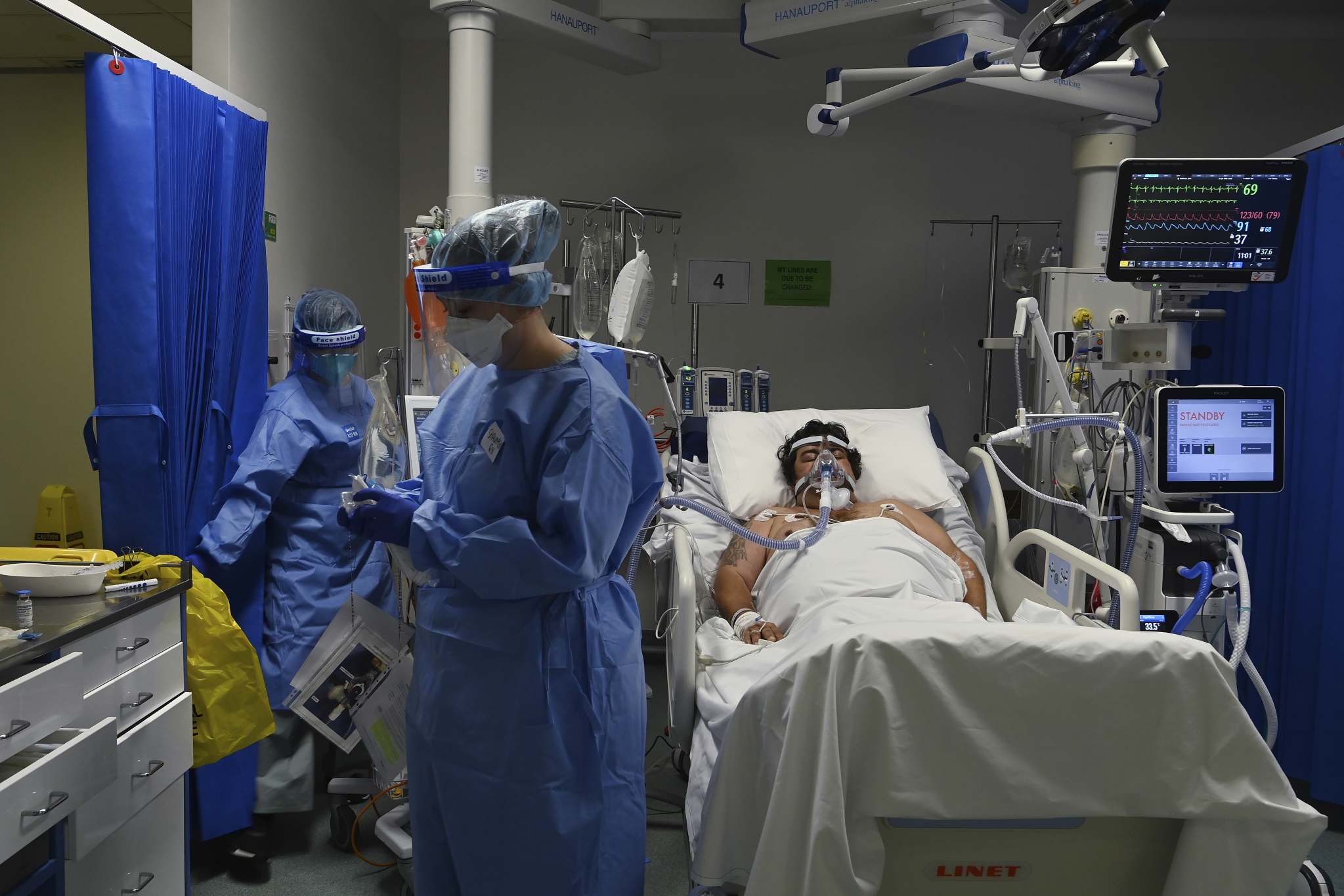

One in three people in the state’s hospitals with COVID-19 is in intensive care, as Sydney’s health system becomes the first in the country to confront the latest wave of highly transmissible Delta-variant cases.
“We are seeing a more diverse group of patients this time, with a disproportionate number of younger patients in ICU,” said Dr Paul Preisz, medical director of the emergency department at St Vincent’s Hospital in Darlinghurst. “It just seems like nobody is safe.
“Last year we saw older patients with high blood pressure and other existing conditions but this time they are younger, with no medical problems. We are seeing a broader range of ages.”
But despite an influx of patients, Dr Preisz said the system was now better at managing the disease through life-saving treatments including the inexpensive steroid dexamethasone, oxygen management and the antiviral remdesivir.
“We are more experienced this time, hundreds of people are now being monitored at home and there is more data out there on how to manage it. We have a more mature system,” said Dr Preisz.
During the peak of the first wave of COVID-19 in April last year NSW recorded about 250 cases in hospital in a single day, of which 40 were in ICU.
There are currently 65 cases in Sydney’s hospitals, including 21 in ICU with four who are ventilated.
The rise in hospitalisations comes as about 1.3 million people in NSW, almost half the population aged over 50, are yet to receive their first dose of the vaccine.
Dr Preisz said there had been a “dramatic change in hospital management”, with double the number of doctors in their dedicated emergency department red zone, an area blocked off for suspected COVID-19 cases. A green zone is allocated for all other patients. All patients suspected of having the virus are given rapid diagnostic tests that return results within an hour, he said.
“The numbers are getting higher so we’ve increased staff to the red zone, we have opened up beds on the ward for COVID-19 positive patients and ICU has expanded to take over other spaces so they can manage. Surgery has been cut back.”
General and vascular surgeon at St Vincent’s Dr Anthony Grabs said the rise in cases is now posing a threat to people needing elective surgery, with beds being carefully monitored every 12 hours to make sure elective surgeries are prioritised based on need.
“We are not stopping elective surgery by any means but patients are voting with their own feet. Some waiting on hip or knee replacements have decided to cancel because the risk is too high,” he said.
“There is only a finite capacity within the system. We have to have the staff. It is all good and well to have operating theatres, but we need the staff.”
NSW’s elective surgery waiting list blew out to more than 100,000 patients in mid-2020 after national cabinet declared a moratorium on non-urgent operations during the first months of the pandemic.
St Vincent’s Hospital is currently caring for about 30 COVID-19 patients via a “hospital at home” or telehealth program as well as another 12 hospital inpatients of which six are in ICU.
“But our protocols, treatment and management of patients have matured a lot,” said Dr Preisz. “And we’re much more aware of treatments than we were a year ago.”
The steroid dexamethasone is the stand-out, shown to bring down the risk of death by a third for COVID patients on ventilators.
“All NSW hospitals have COVID-19 surge plans but St Vincent’s, Liverpool and Westmead have the infrastructure and specialities to do the heavy lifting,” he said.
“Although there are more patients in ICU compared to the first wave there aren’t necessarily more on ventilation and many, many more are monitored at home.”
Of the 767 cases in NSW many are managed via virtual hospitals, by specialists with daily checkups, talking to the patients and examining them over telehealth.
Alan Waitsman tested positive to COVID-19 in late June and was looked after through St Vincent’s virtual care program. His daughter Claudia, 25, contracted the virus at the Joh Bailey salon in Double Bay on June 20.
“I mostly had no symptoms but my daughter had a loss of taste, smell and was short of breath. The hospital managed both of us at home by calling us every day to check on us and we had to report our blood oxygen levels using a finger clip and our blood pressure.”
A second death linked to the outbreak was announced on Monday. It is unclear if the eastern suburbs man, aged in his 70s, was vaccinated.
Dr Kerry Chant urged anyone over the age of 60 to book a vaccination immediately.
“I am urging everyone over 60 to talk to their GP and look at any opportunity to get vaccinated,” she said.
Compared to other states and territories, NSW has the lowest percentage of people aged over 50 and over 70 who have received their first COVID-19 vaccine dose. Almost half the population aged over 50 in NSW (about 1.3 million people) are yet to receive their first dose. About 29 per cent of people over 70 in NSW (280,000) have yet to receive a first dose.
Nationwide, about 43 per cent of people aged over 50 have not yet received their first dose, while among over 70s about 27 per cent have not received their first jab.
Source: smh.com.au




